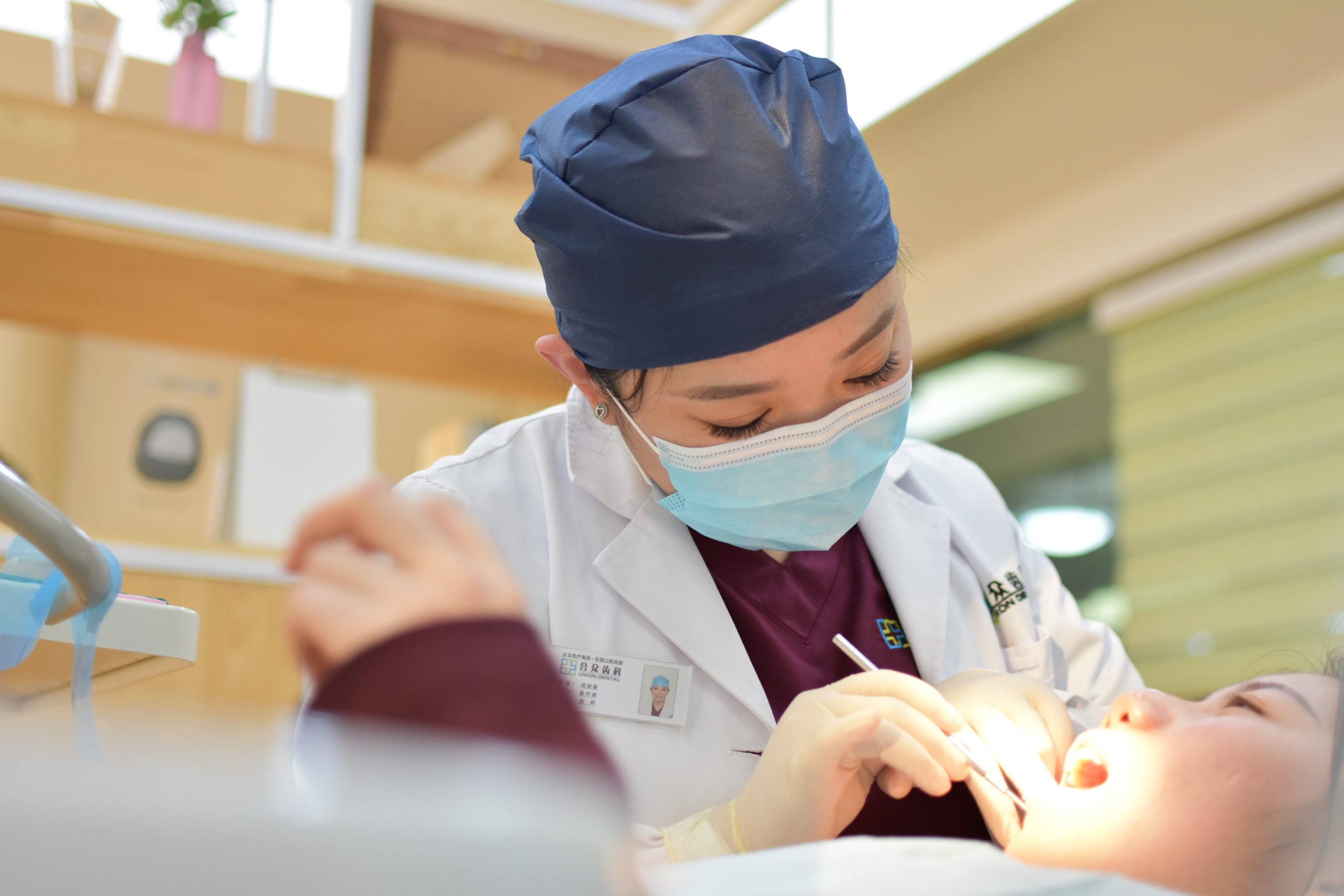
Dental care access in the United States has ebbed to problematic low. According to Pew Trusts, more than 73 million people currently lack dental insurance, while nearly 57 million reside areas without a proportional supply of dentists. Recently-published data from the Health Resources and Service Administration further indicates that there are 6,772 designated dental health professional shortage areas (i.e., regions where there are more than 5,000 patients per dentist) nationwide. These shortages are often more acute in rural areas, given that an estimated two-thirds of dentists practice in population-dense metropolitan areas; however, certain urban communities — particularly those that already face resource shortfalls such as food deserts — do lack access to dental care professionals.
For patients, the consequences of subpar access can be severe. Studies have associated periodontal disease with an increased risk for cancer and cardiovascular conditions. Poor oral care can also contribute to worse health outcomes overall. However, the potential negative results of subpar dental care extends far beyond health alone; if left untreated, dental conditions may impact a patient’s appearance and leave them vulnerable to social stigma and unfavorable judgement in their working and social lives.
The lack of access is a pressing public health issue, and all the more so for its disproportionate impact on low-income communities. Research indicates that those whose incomes are low enough to merit Medicaid enrollment are two times as likely to experience untreated tooth decay when compared to higher-income patients. According to a study published in the Journal of the American Dental Association in 2014, dental conditions accounted for roughly $1 billion in annual emergency department spending, and a full third of all emergency department visits made during the study period were attributed to Medicaid patients.
As one reporter for the New York Times sums up the matter in an article on the subject, “Compared with those enrolled in private coverage through an employer or on their own, the population eligible for Medicaid is much more likely to need dental care and much less likely to be able to afford it or coverage for it.”
This trend is problematic, especially given that a significant portion of dentists do not participate in the public programs that support low-income patients. Medicaid, too, is not perfect; the program has a few significant limitations that exacerbate the current access concern. Currently, federal law does not require Medicaid to provide dental benefits to enrolled adults; instead, it offers at as an option at the state level. Typically, the states that do offer limited dental coverage only pay for extractions or other emergency procedures. Medicare, in comparison, offers no dental benefits at all to its enrollees.
There is little doubt that America’s access shortfall will worsen with time as Baby Boomers age and begin to require care for more dental-related problems. The Bureau of Health Workforce estimates that by 2025, several states will be facing a severe lack of dental care providers. Analysts project that the worst-off will be California, Florida, and New York with shortfalls of 1,234, 1,152, and 1,2024 fewer full-time dentists than needed, respectively.
The lack of dentists — and coverage — for low-income patients is a major public health concern. Given that we are unlikely to gain the thousands of dentists necessary to fill the shortfall or resolve Medicaid’s dental coverage gaps quickly, the healthcare sector has an imperative to seek out other, if partial, solutions.
Dental therapists offer one such limited, if invaluable, measure for relieving some of the demand pressure. Dental therapists are mid-level care providers who specialize in providing routine preventative services such as filling cavities. While not full dentists, these professionals are well-trained; current regulations require dental therapists to graduate from an accredited institution and have a professional license. Their aid could be a crucial part of an overarching strategy to expand dental care to underserved areas at low cost.
Currently, dental therapists are authorized to practice freely in eight states and on tribal lands in Alaska, Idaho, Montana, Oregon, and Washington. At the end of last December, Michigan became the latest state to pass legislation allowing dental therapists to practice. For proponents, passing the bill served as an invaluable way to both support underserved patients and lower costs for public care programs.
As Senator Mike Shirkey, the legislation’s Senate sponsor, commented for Pew, “This bill will ensure an improvement in overall access to oral health care for underserved patients while allowing dentists the chance to expand their practices and increase revenues. Too often, those with limited access to dental care resort to emergency rooms for relief, and Michigan taxpayers have to foot the bill. Creating dental therapists is a solution from both a public health and fiscal perspective.”
Establishing dental therapists is a viable means of expanding access and limiting costs for payers and patients alike. Going forward, states — and those that will face a pressing provider shortfall in the coming years in particular — should consider legislation that would allow dental therapists to practice, if only as a partial solution to America’s current care access problem.